2213
Correlation between imaging features of lenticulostriate artery and cognitive impairment in patients with cerebral small vessel disease1The First Affiliated Hospital of Dalian Medical University, Dalian, China, 2The First Affiliated Hospital of Dalian Medical University,, Dalian, China
Synopsis
Keywords: Blood Vessels, Blood vessels
Motivation: The association between cognitive impairment and lenticulostriate arteries (LSAs) in patients with CSVD remains uncertain.
Goal(s): This study aims to investigate the relationship between the imaging characteristics of lenticulostriate arteries (LSAs) and cognitive function in patients with sporadic CSVD.
Approach: Forty-seven CSVD patients and 28 healthy people were prospectively recruited. According to the MoCA score and years of education, they were divided into the Non-VCI group and the VCI group .
Results: The decrease in the number of LSA was an independent risk factor for VCI in CSVD patients . The number and total length of LSA were significantly correlated with MMSE and MoCA score.
Impact: LSAs is associated with overall cognitive dysfunction in CSVD patients, and the number of LSAS is an independent risk factor for VCI in CSVD patients.
Introduction
cerebral small vessel disease (CSVD) is the most common cause of vascular cognitive impairment (VCI). Visualization of the lenticulostriate artery is essential for understanding the mechanisms of microangiopathy. This study aims to investigate the relationship between the imaging characteristics of lenticulostriate arteries (LSAs) and cognitive function in patients with sporadic CSVD.Methods
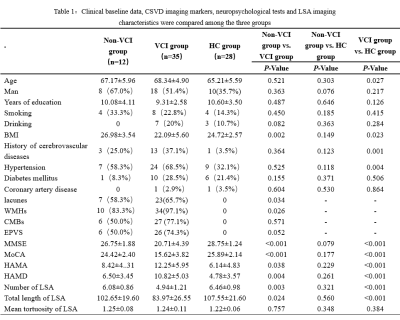
Forty-seven CSVD patients were prospectively recruited, including 26 males and 21 females, aged 60-85 years. According to the Montreal Cognitive Assessment (MoCA) score and years of education, they were divided into the Non-VCI group (12 cases) and the VCI group (35 cases). Healthy elderly people in the same period were selected as the control group (28 cases). All three subject groups underwent magnetic resonance imaging examination, including conventional and high-resolution vascular wall imaging (VWI) sequences, as well as neuropsychological assessments such as the Mini-Mental State Examination (MMSE), Hamilton Anxiety Scale (HAMA), Hamilton Depression Scale (HAMD), and MoCA. Conventional sequences were used to assess the presence of lacune, white matter hyperintensities (WMHs), cerebral microbleeds (CMBs), and enlarged peripheral vascular Spaces (EPVS) in each subject, and VMI sequences were used to measure the number, total length, and mean tortuosity of LSAs. The t-test was employed to compare measurement data between groups, while the χ2-test was utilized for assessing count data between groups. Multivariate logistic regression was employed to investigate the risk factors associated with cognitive dysfunction in CSVD patients. Pearson's or Spearman's correlation was utilized to examine the relationship between the imaging characteristics of the lenticulostriate artery and cognitive dysfunction.Results
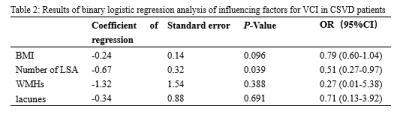
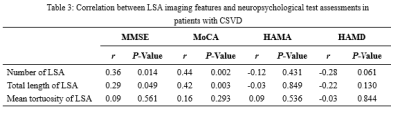
The MMSE, MoCA, the number of LSA and the average length of LSA in the VCI group were significantly lower than those in the non-VCI group and the HC group (all P <0.05); HAMA and HAMD in the VCI group were significantly higher than those in the non-VCI group and the HC group (both P < 0.05); The lacune and WMHs in the VCI group were significantly more than those in the non-VCI group (both P < 0.05, Table 1). The decrease in the number of LSA was an independent risk factor for VCI in CSVD patients (OR = 0.51, 95%CI = 0.27-0.97, P = 0.039; Table 2). The number and total length of LSA were significantly correlated with MMSE (r = 0.36, 0.25, both P < 0.05) and MoCA score (r = 0.44, 0.42, both P < 0.05, Table 3).Conclusion
LSAs is associated with overall cognitive dysfunction in CSVD patients, and the number of LSAS is an independent risk factor for VCI in CSVD patients.Acknowledgements
No acknowledgement found.References
No reference found.Figures