0717
Multi-region Radiomics-based Prediction of Microvascular Invasion in Hepatocellular Carcinoma Using Multi-sequence MRI1Hainan General Hospital (Hainan Affiliated Hospital of Hainan Medical University), Haikou, China, 2Philips Healthcare, Guangzhou, China
Synopsis
Keywords: Liver, Cancer
Motivation: Identifying MVI before surgery is crucial to optimizing treatment strategies and predicting prognosis.
Goal(s): To develop a multi-region radiomics-based predictive model using multi-sequence MRI to assess MVI in HCC.
Approach: Three Models (Tumor, Tumor-Expand5, Tumor-Expand10) were constructed and evaluated.
Results: The Tumor-Expand5 model, with the best predictive accuracy, demonstrates its effectiveness. The research explores the advantages of 5mm VOI expansion for MVI diagnosis over the 10mm VOI expansion, providing valuable insights. Despite limitations, this study offers a preoperative tool to predict MVI in HCC, enhancing clinical decision-making.
Impact: Predicting Microvascular Invasion (MVI) in HCC through multi-region radiomics-based MRI advances precision medicine and treatment optimization. The Tumor-Expand5 model's superior diagnostic performance demonstrates the potential to enhance clinical decision-making.
Introduction
Microvascular invasion (MVI) in hepatocellular carcinoma (HCC) was defined as the presence of cancer cell clusters within a vascular space (mostly in the portal vein, hepatic vein, or a large capsular vessel of the surrounding hepatic tissue) lined by the endothelium, that was visible only by microscopy [1]. Several studies have demonstrated the importance of MVI in the prognosis of patients with HCC [2]. For HCC patients at high risk of MVI, alternative treatment strategies and adjuvant therapy should be considered [3]. Consequently, identifying MVI before surgery is crucial to optimizing the treatment strategy and predicting the prognosis. Radiomics, a newly emerging form of medical image analysis, can obtain high-throughput imaging features for quantitative analysis, advancing precision medicine to a high level [4]. Radiomics-based models have been shown to accurately predict cancer diagnosis, therapeutic efficacy, and prognosis for clinical decision-making [5, 6]. In this study, we aimed to develop a multi-region radiomics-based model using multi-sequence MRI to predict MVI in HCC before operation.Methods
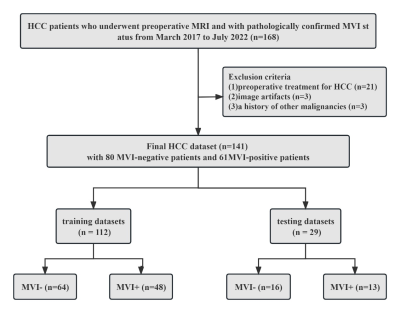
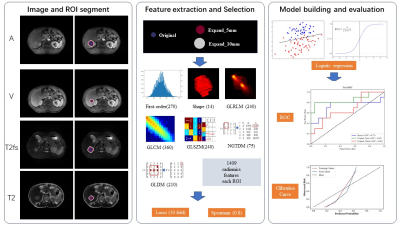
We enrolled 141 HCC patients, including 61 with MVI, diagnosed between March 2017 and July 2022. The patients were randomly divided into training (n = 112, 80%) and testing (n = 29, 20%) groups (see Figure 1). We analyzed four MRI sequences, including T2-weighted imaging (T2WI), T2WI with fat suppression (T2WIfs), arterial phase, and venous phase. For each patient, the tumor volume of interests (VOIs) were manually delineated, with automatic 5mm and 10mm VOI expansions. A total of 1409 radiomic features were extracted from each VOI. Feature selection was performed using the least absolute shrinkage and selection operator (LASSO) and Spearman correlation analysis. Three logistic regression models, namely Tumor, Tumor-Expand5, and Tumor-Expand10, were established based on the radiomic features (see Figure 2). Clinical data were collected and compared using Wilcoxon rank-sum tests or chi-square tests. A combined model, incorporating clinical risk factors and the signature of the optimal radiomics model, was constructed. Model performance was assessed using receiver operating characteristic (ROC) analysis and Delong’s test.Results
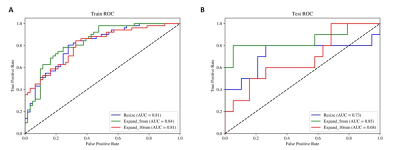
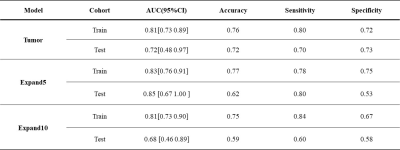
The study included 123 male and 18 female patients, with ages ranging from 30 to 82 years (mean age ± standard deviation: 55.85±10.00 years). We observed significant differences between the MVI and non-MVI groups in terms of Maximum tumor diameter, hepatitis B virus (HBV)-DNA, and Aspartate Aminotransferase (AST). The prediction results of three models (Tumor, Tumor-Expand5, and Tumor-Expand10) are shown in Table 1. Among the three radiomics models, the Tumor-Expand5 model emerged as the top performer. This model exhibited an AUC of 0.83 (95% CI 0.76–0.91) in the training cohort with sensitivity, specificity, and accuracy of 78.4, 75.4, and 76.8% respectively. In the testing cohort, the model yielded an AUC of 0.85 (95% CI 0.67–1.00) with sensitivity, specificity, and accuracy of 80.0, 52.6, and 62.1% respectively. (Figure 3)Discussion
MVI often occurs in peritumoral tissue, whose vessels also serve as a pathway for hematogenous dissemination of portal vein tumors [7, 8]. Thus, many studies related to microvascular invasion in hepatocellular carcinoma tend to expand VOI [9, 10, 11]. However, the expansion of VOI can vary widely, ranging from 1mm to 10mm, and there is no consensus on the optimal range. For this reason, we constructed multi-VOI models to investigate this highly aggressive area. Interestingly, the AUC of VOITumor-Expand5 was superior to the VOITumor model in predicting MVI risk grades. These preponderances of tumor expansions for predicting MVI align with some previous studies. Up to now, no research has been reported about the comparison of 5mm and 10mm VOI expansions in predicting MVI of HCC from multi-sequence MRI. It’s noteworthy that our research found that the Tumor-Expand5 model possesses an advantage over the Tumor-Expand10 model. This suggests that the radiomic features of the 5mm expansions from the tumor contribute more to the diagnosis of MVI in HCC than the 10mm expansions from tumor. This study has several limitations. Firstly, this is a retrospective single-center study that needs to be further prospectively validated with larger cohorts within multi-center studies. Secondly, variations in tumor VOI outlines across different sequences may exist due to manual delineation. In future research, more accurate and automated tumor segmentation techniques should be considered to enable in-depth analysis.Conclusion
In conclusion, multi-region radiomics from multi-parametric MRI have diverse effects for predicting MVI in patients with HCC. Our final preoperative prediction model, mainly based on multi-parametric MRI radiomics in VOITumor-Expand5 is a preoperative tool for predicting MVI in patients with HCC, potentially enhancing clinical decision-making.Acknowledgements
No acknowledgement found.References
[1] Sheng X, Ji Y, Ren GP, et al. A standardized pathological proposal for evaluating microvascular invasion of hepatocellular carcinoma: a multicenter study by LCPGC. Hepatol Int. 2020;14(6):1034-1047. doi:10.1007/s12072-020-10111-4
[2] Lei Z, Li J, Wu D, et al. Nomogram for Preoperative Estimation of Microvascular Invasion Risk in Hepatitis B Virus-Related Hepatocellular Carcinoma Within the Milan Criteria. JAMA Surg. 2016;151(4):356-363. doi:10.1001/jamasurg.2015.4257
[3] Omata M, Cheng AL, Kokudo N, et al. Asia-Pacific clinical practice guidelines on the management of hepatocellular carcinoma: a 2017 update. Hepatol Int. 2017;11(4):317-370. doi:10.1007/s12072-017-9799-9
[4] Gillies RJ, Kinahan PE, Hricak H. Radiomics: Images Are More than Pictures, They Are Data. Radiology. 2016;278(2):563-577. doi:10.1148/radiol.2015151169
[5] Bera K, Braman N, Gupta A, Velcheti V, Madabhushi A. Predicting cancer outcomes with radiomics and artificial intelligence in radiology. Nat Rev Clin Oncol. 2022;19(2):132-146. doi:10.1038/s41571-021-00560-7
[6] Hu H, Zheng Q, Huang Y, et al. A non-smooth tumor margin on preoperative imaging assesses microvascular invasion of hepatocellular carcinoma: A systematic review and meta-analysis. Sci Rep. 2017;7(1):15375. Published 2017 Nov 13. doi:10.1038/s41598-017-15491-6
[7] Roayaie S, Blume IN, Thung SN, et al. A system of classifying microvascular invasion to predict outcome after resection in patients with hepatocellular carcinoma. Gastroenterology. 2009;137(3):850-855. doi:10.1053/j.gastro.2009.06.003
[8] Qu C, Wang Q, Li C, et al. A Radiomics Model Based on Gd-EOB-DTPA-Enhanced MRI for the Prediction of Microvascular Invasion in Solitary Hepatocellular Carcinoma ≤ 5 cm. Front Oncol. 2022;12:831795. Published 2022 May 19. doi:10.3389/fonc.2022.831795
[9] Zhang X, Ruan S, Xiao W, et al. Contrast-enhanced CT radiomics for preoperative evaluation of microvascular invasion in hepatocellular carcinoma: A two-center study. Clin Transl Med. 2020;10(2):e111. doi:10.1002/ctm2.111
[10] Feng ST, Jia Y, Liao B, et al. Preoperative prediction of microvascular invasion in hepatocellular cancer: a radiomics model using Gd-EOB-DTPA-enhanced MRI. Eur Radiol. 2019;29(9):4648-4659. doi:10.1007/s00330-018-5935-8
[11] Zhang R, Xu L, Wen X, et al. A nomogram based on bi-regional radiomics features from multimodal magnetic resonance imaging for preoperative prediction of microvascular invasion in hepatocellular carcinoma. Quant Imaging Med Surg. 2019;9(9):1503-1515. doi:10.21037/qims.2019.09.07
Figures