4604
Combined hepatocellular-cholangiocarcinoma: diagnostic and prognostic values of LI-RADS v2017 categorization on gadoxetic acid-enhanced MR imaging1Seoul National University Hospital, Seoul, Republic of Korea, 2Hallym University Sacred Heart Hospital, Anyang, Republic of Korea
Synopsis
Our retrospective study investigated the utility of Liver Imaging Reporting and Data System (LI-RADS) v2017 for combined hepatocellular cholangiocarcinoma (cHCC-CCs) in the differential diagnosis from HCCs and prediction of prognosis. Using LI-RADS on gadoxetic acid-enhanced MRI, among cHCC-CCs (n=70), 61.4% (43/70) were accurately categorized as LR-M (probable malignancy, not specific for HCC) while 37.1% (26/70) as LR-5/4 (definitely/probably HCC); among HCCs (n=70), 88.6% (62/70) and 10.0% (7/70) were categorized as LR-5/4 and LR-M, respectively. After surgical resection, patients with LR-M cHCC-CCs showed a higher early recurrence rate (≤6 months) than those with LR-5/4 cHCC-CCs (27.8% (10/36) vs. 4.8% (1/21), P=0.041).
Introduction
Combined hepatocellular cholangiocarcinoma (cHCC-CC) is a rare form of primary liver cancer consisting of mixed elements of hepatocellular carcinoma (HCC), cholangiocarcinoma (CC), and/or components with hepatic stem cell features which is predominantly developed in patients with liver cirrhosis or chronic viral hepatitis. Imaging differentiation of cHCC-CCs from HCCs is often challenging but clinically important because of differences in treatment strategies and prognosis.1-4 The liver imaging reporting and data system (LI-RADS), recently updated in 2017, provides tools for standardizing the imaging diagnosis of HCC in patients at high risk for HCC.5 In addition to scoring the likelihood of HCC, it also includes a special category for observations that are probably malignant but are not specific for HCC, namely LR-M, intending to preserve specificity for diagnosis of HCC while not losing sensitivity for diagnosis of malignancy. In this study, we aimed to investigate the utility of LI-RADS v2017 for cHCC-CCs on gadoxetic acid-enhanced MRI in the differential diagnosis from HCCs and prediction of prognosis.Methods
This retrospective study was approved by our Institutional Review Board with waiver of informed consent. We included patients at high risk for HCC with pathologically confirmed cHCC-CCs (n=70) and a matched control group of HCCs (n=70) who had undergone gadoxetic acid-enhanced MRI. For each cHCC-CC or HCC, MR imaging features were assessed and LI-RADS categories were assigned by using a consensus-based interpretation of three radiologists. Diagnostic performances of LR-M (probable malignancy, not specific for HCC) for the differential diagnosis of cHCC-CCs from HCCs were investigated, and imaging features were compared between cHCC-CCs of LR-M and those of LR-5/4 (definitely/probably HCC). Among patients who had undergone surgical resection for cHCC-CCs, early recurrence rates within 6 months after surgery were compared between LR-M and LR-5/4.Results
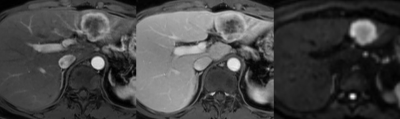
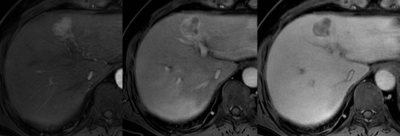
Using LI-RADS, cHCC-CCs were categorized as LR-M in 61.4% (43/70), LR-5/4 in 37.1% (26/70), and LR-TIV (tumor in vein) in 1.4% (1/70), respectively; whereas HCCs were categorized as LR-M in 10.0% (7/70), LR-5/4 in 88.6% (62/70), and LR-TIV in 1.4 % (1/70), respectively. When comparing MR imaging features between cHCC-CCs of LR-5/4 (n=26) and those of LR-M (n=43), cHCC-CC of LR-5/4 showed significantly higher frequencies of major HCC features including arterial hyper-enhancement (96.2% (25/26) vs. 58.1% (25/43), P=0.001), washout appearance (80.8% (21/26) vs. 48.8% (21/43), P=0.011), and capsule appearance (34.6% (9/26) vs. 11.6% (5/43), P=0.031), while showed lower frequencies of non-HCC malignancy-favoring features such as arterial phase peripheral enhancement (0% (0/26) vs 68.9% (30/43), P<0.001), hepatobiliary phase target appearance (3.7% (1/26) vs. 58.1% (25/43), P<0.001) and liver surface retraction (0% (0/26) vs. 16.3% (7/43), P=0.040) than cHCC-CCs of LR-M. Among patients with cHCC-CCs who underwent curative surgery (n=57), early recurrence rate within 6 months was significantly higher in patients with cHCC-CCs of LR-M than those with cHCC-CCs of LR-5/4 (27.8% (10/36) vs. 4.8% (1/21), P=0.041).Discussion
In this study, although 61.4% of cHCC-CCs were accurately categorized as category LR-M using the latest LI-RADS on gadoxetic acid-enhanced MRI, substantial proportion of cHCC-CCs were categorized as LR-5/4 (37.1%). In other words, cHCC-CC can be a cause of lowering the specificity of HCC diagnosis by using LI-RADS. On gadoxetic acid-enhanced MRI, cHCC-CCs of LR-5/4, i.e. HCC mimickers, showed higher frequencies of major HCC features and lower frequencies of non-HCC malignancy-suggestive findings than those of LR-M. This heterogeneity in imaging features may reflect the diversity in proportions of histologic components. A recent study reported that hypervascular cHCC-CC on MRI would have larger HCC component pathologically, while non-hypervascular cHCC-CC would have larger CC component.6 Our study showed the potential value of LI-RADS in the prognostic stratification: cHCC-CCs of LR-M showed higher early recurrence rate compared with those of LR-5/4. While cHCC-CCs are reported to have worse prognosis than HCCs, it can be different according to subgroups of cHCC-CCs considering our study results in surgical outcomes. Further studies for long-term outcomes of cHCC-CCs in comparison of HCCs of same LI-RADS categories would be needed to more understand the clinical significance of LI-RADS categorization.Conclusion
Using LI-RADS on gadoxetic acid-enhanced MRI, a considerable proportion of cHCC-CCs can be misclassified as non-LR-M including LR-5, resulting in a false-positive diagnosis of HCC. In addition, cHCC-CC mimicking HCC (LR-5/4) may show better surgical outcomes in regards to early recurrence than cHCC-CC of LR-M.Acknowledgements
No acknowledgement found.References
1. Potretzke TA, Tan BR, Doyle MB, Brunt EM, Heiken JP, Fowler KJ. Imaging Features of Biphenotypic Primary Liver Carcinoma (Hepatocholangiocarcinoma) and the Potential to Mimic Hepatocellular Carcinoma: LI-RADS Analysis of CT and MRI Features in 61 Cases. AJR American journal of roentgenology 2016;207(1):25-31.
2. Sapisochin G, Fidelman N, Roberts JP, Yao FY. Mixed hepatocellular cholangiocarcinoma and intrahepatic cholangiocarcinoma in patients undergoing transplantation for hepatocellular carcinoma. Liver transplantation : official publication of the American Association for the Study of Liver Diseases and the International Liver Transplantation Society 2011;17(8):934-942.
3. Yin X, Zhang BH, Qiu SJ, et al. Combined hepatocellular carcinoma and cholangiocarcinoma: clinical features, treatment modalities, and prognosis. Annals of surgical oncology 2012;19(9):2869-2876.
4. Jung DH, Hwang S, Song GW, et al. Longterm prognosis of combined hepatocellular carcinoma-cholangiocarcinoma following liver transplantation and resection. Liver transplantation : official publication of the American Association for the Study of Liver Diseases and the International Liver Transplantation Society 2017;23(3):330-341.
5. Mitchell DG, Bruix J, Sherman M, Sirlin CB. LI-RADS (Liver Imaging Reporting and Data System): summary, discussion, and consensus of the LI-RADS Management Working Group and future directions. Hepatology (Baltimore, Md) 2015;61(3):1056-1065.
6. Park SH, Lee SS, Yu E, et al. Combined hepatocellular-cholangiocarcinoma: Gadoxetic acid-enhanced MRI findings correlated with pathologic features and prognosis. Journal of magnetic resonance imaging : JMRI 2016.
Figures