4354
A Comparison of Hyperpolarized Helium-3 and Xenon-129 MR Fractional Ventilation Imaging1Radiology, University of Pennsylvania, Philadelphia, PA, United States, 2Anesthesiology and Critical Care, University of Pennsylvania, Philadelphia, PA, United States
Synopsis
In response to the global shortage of 3He, we studied the feasibility and safety of performing a multi-breath wash-in MR imaging technique to measure fractional ventilation using hyperpolarized (HP) 129Xe in the same manner as with 3He.
Introduction
In response to the global shortage of 3He, we studied the feasibility of performing a multibreath wash-in MR imaging technique to measure fractional ventilation using hyperpolarized (HP) 129Xe in the same manner as with 3He1. If HP 129Xe is to be used in the future to accurately assess regional fractional ventilation in human lungs, testing on larger mammals is first necessary to determine its safety and practicality. In this study, results of HP 129Xe and HP 3He fractional ventilation MR imaging in rabbits were compared to determine the potential clinical effectiveness of the former.
Material and Methods
Imaging experiments were performed in five New Zealand rabbits (approx. 4.5 kg) sedated with Propofol. Rabbits were ventilated with room air at two different tidal volumes (6 and 10 ml/kg) using a house-made ventilator shown in Figure 1; during imaging, the ventilator was switched to a normoxic mixture of 129Xe. The tidal volume and inspired oxygen and mixed-expired gasses were analyzed real-time (Biopac, USA) for higher precision in the fitting process1. Imaging was performed in a whole body 1.5-T MRI system (Siemens MAGNETOM) using two quadrature volume coil designed for rabbits tuned to helium and xenon frequency(Stark, Germany).
The fractional ventilation image series consisted of 6 wash-in followed by a final long breath-hold for T1 and flip angle correction, as previously presented1. A 2D multi-slice GRE image set was employed, with 3 ~10 mm coronal slices (adjusted to cover the whole lung with a 20% inter-slice gap), MS=3x64x48 (~3x3 mm2 planar resolution), α=6°, TR/TE=7.0/3.3 ms in case of helium studies and TR/TE=9.0/4.1 ms for xenon. Imaging acceleration was performed using GRAPPA (~2x). Animals were imaged with both gases back-to-back with minimum time between the sessions; the order of imaging with helium and xenon was changed between experiments in different rabbits to reduce bias. An atlas of the lung was generated by summing all the existing data and applying a smoothing Gaussian filter, and all lungs were then registered to the lung atlas. To account for minor position changes during the sequence, and position changes after changing the coils, a non-rigid affine-based co-registration was performed before fitting on spin density maps from all seven time-points. Automatic contrast-limited adaptive histogram equalization with a gray-scale threshold was applied to mask background noise and segment the lung. Image analysis was performed based on the fitting process presented before1. Imaging results with the two gases were compared globally and regionally in both low and high regimes. Imaging gases were polarized up to ~40-50% and ~25-30% for 129Xe polarizer (XeBox, XeMed, USA) and 3He polarizer (Polareon, USA), respectively.
Results and Discussion
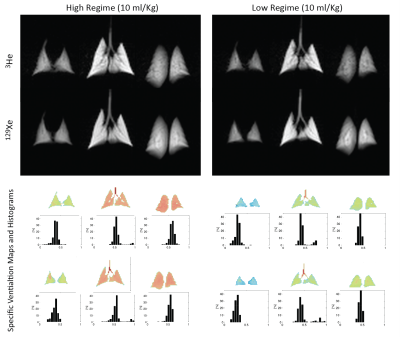
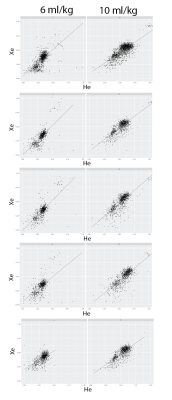
Figure 2 shows the spin density and resulting fractional ventilation maps and histogram of all the three slices for both 3He and 129Xe and both high and low tidal volumes for one representative rabbit. All rabbits tolerated the 7 back-to-back wash-ins of normoxic xenon breaths and the long breath-hold very well, though a slight elevation in heart rate (up to 200 bpm) and a small drop in SpO2 was observed (never less than 93%) in some of the experiments after the lung breath-hold. Overall fractional ventilation measured with 129Xe was 0.278±0.035 and 0.517±0.073 for low and high regimes, respectively, compared to 0.264±0.060 and 0.521±0.068 when measured with 3He. No bias was observed in fractional ventilation calculations using xenon or helium in case of healthy rabbits imaged in this study. Achieving a higher xenon polarization level (100% higher) partially compensated for the lower signal-to-noise when compared with helium (three times higher). Pixel-by-pixel correlation plots for all the rabbits and all the measurements (low and high tidal volume) are shown in Figure 3. Pixel-by-pixel 3He/129Xe correlation for all voxels in all rabbits and both regimes was 0.78±0.18. No systematic bias was observed in pixel values after T1 correction when comparing either 3He or 129Xe or low and high regime.Conclusion
This study compared estimations of regional fractional ventilation obtained with HP 3He and 129Xe, showing a good agreement between the two measurements. It should be noted, however, that the ratio of imaging gas should be reduced to 30% for any future 129Xe human studies; this will result in lower signal-to-noise and produce broader fractional ventilation histograms.Acknowledgements
No acknowledgement found.References
[1] Hamedani H, Clapp JT, Kadlecek SJ, et al. Regional fractional ventilation by using multibreath wash-in 3He MR imaging. Radiology 279 (3), 917-924Figures