2500
Automated Volumetry-based Morphometry in Postural Instability Gait Disorder1Singapore General Hospital, Singapore, Singapore, 2Advanced Clinical Imaging Technology, Siemens Healthcare HC CEMEA SUI DI PI, Lausanne, Switzerland, 3Department of Radiology, University Hospital (CHUV), Lausanne, Switzerland, 4LTS5, École Polytechnique Fédérale de Lausanne, Lausanne, Switzerland, 5Advanced Clinical Imaging Technology, Siemens Healthcare HC CEMEA SUI DI PI, Singapore, Singapore, 6National Neuroscience Institute, Singapore
Synopsis
Postural instability gait disorder (PIGD) subtype in Parkinson's disease (PD) is a major cause of morbidity. We quantified whole-brain structural changes in PIGD patients, PD patients and controls using an automated volume-based morphometry algorithm that is objective and reproducible. Compared to PD and controls, PIGD subgroup demonstrated a significant decrease in brain and globus pallidus volume, as well as grey matter content in both caudate and thalamus; but an increase in ventricular size, abnormal white matter volume and relative caudate size. MRI findings also correlate with gait imbalance severity in PIGD, suggesting a mechanism of temporal differences in segmental volume loss.
Purpose
Postural instability gait disorder (PIGD), a subtype of Parkinson's disease (PD) with rapid progression of disease and cognitive dysfunction, is a major cause of morbidity in advanced disease, but unfortunately not well researched.1 Studies typically quantify neuro-degeneration in the nigro-striatal pathways.2,3 Nonetheless, changes are not limited to these4, and extend to other structures even early on. Automated volume-based morphometry (Vol-BM) analysis is increasingly used to characterize microstructural changes in pathology. We evaluated if Vol-BM is capable of identifying brain changes that differentiate and aid in classifying the PD and PIGD subtypes.Methods
We examined a case-control cohort of 58 subjects, including 20 PD patients, 18 PIGD patients and 20 demographically-matched healthy controls. Whole-brain imaging on 3Tesla MR scanner (Magnetom Trio, Siemens, Erlangen, Germany) was performed, including 3D MPRAGE series: TR/TI 2200/900ms; 240cm FOV; 256x256 matrix; 0.9mm slice thickness; 192 slices.
Automated segmentation of brain structures was performed on MPRAGE images and completed with the MorphoBox prototype software.5 Deep grey nuclei volumes were computed by summing up grey matter (GM) and white matter (WM) probabilities over the relevant masks. WM abnormalities were detected by thresholding the difference between the posterior and prior probability maps,5 according to a constant value of 0.6. For inter-subject comparison, all estimated volumes are normalized based on total brain volume.
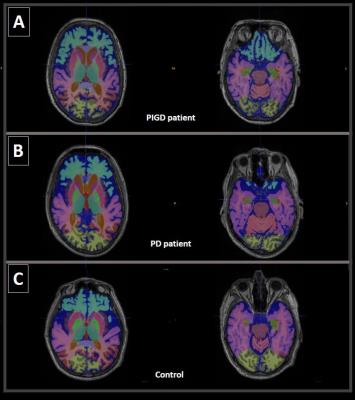
All segmentation masks were viewed using ITK-Snap6 (Figure 1). Quality of segmentation masks were reviewed by two individuals trained in neuroanatomical landmarks, in correlation with corresponding T2-FLAIR images and accompanying clinical neuroradiological reports. Hence, two PIGD patients were excluded due to significant misclassification of GM lesions in the basal ganglia. Neurological and neuropsychological parameters were evaluated using the Hoehn and Yahr scale (HY), Tinetti Balance Scale (TBS) and Mini–Mental State Examination (MMSE). Vascular risk factors were also recorded.
Data analysis was performed using R 3.3.17 at a significance level of 0.05. Kruskal–Wallis test with Bonferroni-corrected pairwise comparisons was used to assess significant brain segmentation and clinical parameter differences across subgroups. Subsequently, after variable selection by stepwise regression, a multivariate regression model, controlled by age and gender, was utilized to assess the relationship between extracted volumetry and clinical scores.
Results
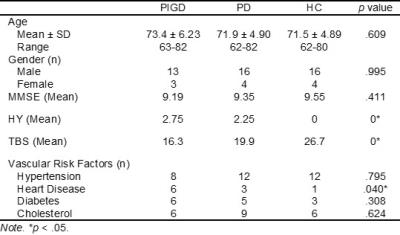
Table 1 shows summarized subject clinico-demographics. Clinically, HY and TBS assessments showed statistically significant pairwise differences across all subgroups. Cranium size was not significantly different across all subgroups. Absolute ventricular (p < .05) and abnormal WM (p < .0001) volumetry were significantly higher in PIGD, compared to PD and controls. Controlling for differences in brain volume, in PIGD, decrease in percentage of GM in both caudate and thalamus, as well as, the decrease in globus pallidus (GP) volumetry were statistically significant (p <.05). Univariate regressions against volumetric data demonstrated significance of GM% in thalamus and caudate, and relative size of caudate in predicting TBS scores (p < .05). Multivariate regression on the whole cohort showed that relative size of the caudate alone significantly predicted TBS scores, b = -2721, t(51) = -4.822, p < .0001. Relative size of the caudate also explained 31% of the of variance in TBS scores, R2 = .31, F(4, 51) = 7.26, p < .0001.Discussion
Conventional MRI findings correlate well with severity of gait imbalance in PIGD, but less so with PD. The decrease in GM% in both caudate and thalamus, along with decrease in GP volumetry, represents neuronal loss in key relay nuclei of the nigrostriatal pathway in PIGD patients. WM abnormalities, especially in the periventricular areas, are also known to be more prevalent in PIGD than in PD and controls.8
Compared to controls, there is an increase in relative caudate volume in PD and PIGD. Despite accounting for segmentation artifacts, this trend reached statistical significance in the PIGD subgroup. This may be explained by temporal differences in volume loss, namely progressive global brain atrophy preceding caudate atrophy.9,10 Obtaining accurate structural measurements from automated segmentation algorithms remains a key technical challenge in such pathological context. That is, some misclassification of periventricular WM lesions and gliotic hypointensities as GM was noted. Partial volume effects of the former contributed to GM concentration of the caudate. Nevertheless, the extent of volume overestimation was less than 1% in the affected images.
Conclusion
Vol-BM allows a viable, objective, consistent and unbiased characterization of structural brain changes in PD and PIGD. Volumetry-based analysis could complement clinical assessment of gait imbalance, and a volumetry-based classification of PIGD patients is potentially possible with further validation. Additionally, we propose a multimodal segmentation that incorporates other relevant sequences (e.g. T2-FLAIR) and additional tissue classes (e.g. abnormal GM) to more accurately account for all brain lesions.Acknowledgements
We thank the National Medical Research Council and Siemens for their support.References
1. Burn DJ, Rowan EN, Allan LM, Molloy S, O’Brien JT, McKeith IG. Motor subtype and cognitive decline in Parkinson’s disease, Parkinson’s disease with dementia, and dementia with Lewy bodies. Journal of Neurology, Neurosurgery, and Psychiatry. 2006;77(5):585-589. doi:10.1136/jnnp.2005.081711.
2. Hutchinson M, Raff U. Structural Changes of the Substantia Nigra in Parkinson's Disease as Revealed by MR Imaging. American Journal of Neuroradiology. April 1, 2000 2000;21(4):697-701.
3. Nagae LM, Honce JM, Tanabe J, Shelton E, Sillau SH, Berman BD. Microstructural Changes within the Basal Ganglia Differ between Parkinson Disease Subtypes. Frontiers in Neuroanatomy. 2016;10:17. doi:10.3389/fnana.2016.00017.
4. Henderson JM, Carpenter K, Cartwright H, Halliday GM. Loss of thalamic intralaminar nuclei in progressive supranuclear palsy and Parkinson's disease: clinical and therapeutic implications. Brain. 2000;123(7):1410-1421.
5. Schmitter D, Roche A, Maréchal B, et al. An evaluation of volume-based morphometry for prediction of mild cognitive impairment and Alzheimer’s disease. NeuroImage : Clinical. 2015;7:7-17. doi:10.1016/j.nicl.2014.11.001.
6. Paul A. Yushkevich, Joseph Piven, Heather Cody Hazlett, Rachel Gimpel Smith, Sean Ho, James C. Gee, and Guido Gerig. User-guided 3D active contour segmentation of anatomical structures: Significantly improved efficiency and reliability. Neuroimage 2006 Jul 1;31(3):1116-28.
7. R Core Team (2013). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. ISBN 3-900051-07-0, URL http://www.R-project.org/.
8. Bohnen NI, Albin RL. White matter lesions in Parkinson disease. Nature Reviews Neurology. 2011;7(4):229-236. doi:10.1038/nrneurol.2011.21.
9. Kish SJ, Shannak K, Hornykiewicz O. Uneven Pattern of Dopamine Loss in the Striatum of Patients with Idiopathic Parkinson's Disease. New England Journal of Medicine. 1988;318(14):876-880.
10. Almeida OP, Burton EJ, McKeith I, Gholkar A, Burn D, O’Brien JT. MRI Study of Caudate Nucleus Volume in Parkinson’s Disease with and without Dementia with Lewy Bodies and Alzheimer’s Disease. Dementia and Geriatric Cognitive Disorders. 2003;16(2):57-63.