2384
Effects of cumulative non-concussive head impact exposure associated with youth football on MRI measures of gray matter structure1Radiology, Wake Forest School of Medicine, Winston Salem, NC, United States, 2Biomedical Engineering, Wake Forest School of Medicine, 3Radiology, University of Texas Southwestern Medical Center, 4Biostatistical Sciences, Wake Forest School of Medicine, 5Radiology & Biomedical Engineering, Wake Forest School of Medicine, 6Family and Community Medicine, Wake Forest School of Medicine, 7Neurosurgery, Wake Forest School of Medicine, 8Radiology, Biomedical Engineering, and Clinical and Translational Sciences Institute, Wake Forest School of Medicine
Synopsis
Millions of children play American football, however, youth players are largely absent from studies addressing the public health questions about safety and concussion. Furthermore, many studies investigating effects of sports-related head impact exposure on brain structure have focused on white matter, with few evaluating the effects on gray matter (GM) structure. In this study, we combined measures of head impact biomechanics and brain MRI to investigate the effects of repetitive non-concussive exposure on gray matter volume and microstructural integrity. We demonstrate statistically significant relationships between exposure metrics and MRI measures of GM diffusion characteristics after one season of youth football.
Introduction:
The purpose of this work was to investigate the effects of sports-related non-concussive head impact exposure on GM structure in children engaged in American football by combining head impact biomechanics and brain MRI. Another purpose was to compare MRI measures of GM structure using standard volumetrics with diffusion kurtosis imaging (DKI) measures of GM microstructural integrity, which has been shown to be sensitive to developmental changes in the brain.1 Our overall hypothesis was that there would be statistically significant linear relationships between cumulative head impact exposure and changes in GM structure after one season of youth football, with stronger associations for DKI measures compared to standard GM volumetrics.Methods:
Head impact exposure data was obtained from 22 youth male football players (ages 10-14) using the Head Impact Telemetry System (HITS) during all practices and games. None of the players had a history of neurological or psychiatric disease, and none had a history of concussion before or during the football season. Participants received pre- and post-season neuroimaging with MRI from which measures of GM volume and diffusion characteristics were acquired using a standard high-resolution isotropic T1-weighted sequence and DKI, respectively. To investigate changes over the season for each player, quantitative metrics from pre-season MRI were subtracted from post-season MRI. A z-score analysis was then used to obtain a total number of abnormal GM voxels, defined as 2 standard deviations above or below the group mean, from the post- minus pre-season MRI measures. Risk weighted cumulative exposure (RWE) was computed from HITS data, including combined probability (RWECP) that encompasses both linear and rotational components.2 This metric represents the cumulative risk of concussion over the course of the season. Several metrics, including RWECP, GM volume, mean diffusivity, mean kurtosis, axial diffusivity, and radial diffusivity, were skewed and were log transformed to meet the assumptions of normality. Linear regression analyses were conducted to assess the relationship between RWECP and post-pre MRI measures of GM volume and diffusion characteristics. Cooks distance was computed to identify and exclude outliers for each analysis.Results:
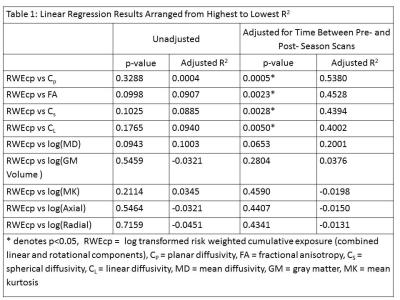
Regression analyses adjusted for time between pre- and post- season MRI scans demonstrated a statistically significant linear relationship between RWECP and the number of abnormal GM voxels for several diffusion metrics (Table 1). Of the diffusion metrics analyzed, planar diffusivity explained the most variance (Figure 1). There was no statistically significant relationship between RWECP and GM volume.Discussion:
This study demonstrates a statistically significant linear relationship between cumulative head impact exposure and number of abnormal voxels from measures of diffusion characteristics in GM after one season of football in youth players. These changes were primarily associated with FA and its subcomponents, including linear, planar, and spherical diffusivity, with planar explaining the most variance. Planar explaining the most variance may reflect disruption of the unique microstructural architecture of gray matter, but further work is necessary to explore the potential underlying pathophysiology. FA seems to be an important measure to detect change in both GM and WM.3-4 Changes in GM FA after mild traumatic brain injury (mTBI) have been shown to be associated with glial cell migration and cytotoxic edema.5 It was necessary to adjust for time between MRI scans to reveal significant linear relationships. This suggests the need to control for variability associated with brain development in this age group undergoing rapid maturation. It is important to note that several factors limit the generalizability of our results to the overall population of youth athletes, including the relatively small sample size, single sex (males) and focus on American football. More research using a larger sample size, variety of contact/semi-contact sports, and a longitudinal design will be necessary to determine whether these changes are 1) reproducible, 2) transient or long-standing, and 3) progressive in a dose-dependent way with additional seasons of play.Conclusion:
We found that cumulative head impact exposure over a single season of youth football was associated with changes in GM microstructural integrity, as measured with diffusion MRI, but not GM volume. These changes were present in youth footballers without the clinical diagnosis of concussion, suggesting that even so-called “subconcussive” head impacts may be biologically relevant with respect to the developing brain. These findings also suggest that measures of microstructural integrity via diffusion MRI may be more sensitive than simple volumetric measurements for detecting changes in GM associated with repetitive head impact exposure.Acknowledgements
Supported by Childress Institute for Pediatric Trauma at Wake Forest School of Medicine and National Institutes of Health (NINDS R01NS082453 and R01NS091602).References
1. Davenport EM, Kalyna A, Whitlow CT, et al. Abnormalities in Diffusional Kurtosis Metrics Related to Head Impact Exposure in a Season of High School Varsity Football. Journal of Neurotrauma. Published online: 2016 May 18. doi:10.1089/neu.2015.4267.
2. Urban JE, Davenport EM, Golman AJ, et al. Head Impact Exposure in Youth Football: High School Ages 14 to 18 Years and Cumulative Impact Analysis. Annals of biomedical engineering. 2013;41(12):2474-2487. doi:10.1007/s10439-013-0861-z.
3. Y. Chun, X. Mao, E.L. Breedlove, L.J. Leverenz, E.A. Nauman & T.M. Talvage (2015) DTI Detection of Longitudinal WM Abnormalities Due to Accumulated Head Impacts. Developmental Neuropsychology. 40:2, 92-97, DOI: 10.1080/87565641.2015.1020945
4. Talavage TM, Nauman EA, Leverenz LJ. The Role of Medical Imaging in the Recharacterization of Mild Traumatic Brain Injury Using Youth Sports as a Laboratory. Frontiers in Neurology. 2015;6:273. doi:10.3389/fneur.2015.00273.
5. Budde MD, Janes L, Gold E, Turtzo LC, Frank JA. The contribution of gliosis to diffusion tensor anisotropy and tractography following traumatic brain injury: validation in the rat using Fourier analysis of stained tissue sections. Brain. 2011;134(8):2248-2260. doi:10.1093/brain/awr161.
Figures